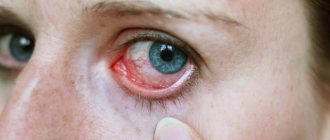
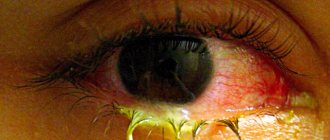
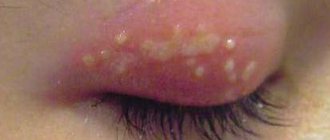
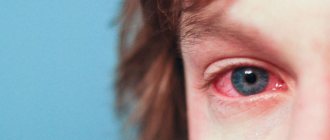
The term conjunctivitis refers to inflammation of the conjunctiva of the eye. This disease is especially common in childhood due to the fragile immune system. The most common purulent conjunctivitis in children is accompanied by copious discharge. What are the causes and treatment of this pathology?
Causes
In children, the purulent form of the disease is more common than in adults. There is only one cause of the disease - exposure to a bacterial infection (gonococci, chlamydia, nonspecific flora: Pseudomonas aeruginosa, streptococci, staphylococci, Klebsiella).
Most often, infection occurs under the influence of the following factors:
- unstable immune defense in a child;
- failure to comply with hygiene measures;
- frequent injury to the conjunctiva.
Transmission of infection occurs in different ways:
- through contact of a healthy person with a sick person, rubbing the eyes with dirty hands;
- when swimming in public bodies of water;
- through coughing or sneezing;
- damage to the fetus in utero or during the baby’s passage through the birth canal. It happens if the mother has untreated gynecological diseases.
Therapy for eye infection with chlamydia
Chlamydial conjunctivitis is a disease also characteristic of newborns. Infection occurs during childbirth through direct contact of the baby with the mother’s diseased birth canal. The disease may appear 5-7 days after birth.
In comparison with the more acute course of the disease in adults, the general clinical picture in a child is:
- excessive tearing;
- discharge of mucopurulent secretion of a yellow or greenish tint;
- redness of the whites of the eyes.
If you do not start saving the baby’s visual organs, the prognosis for the disease is not the most favorable. Eyelid deformation and keratitis are the most common complications of chlamydial infection, which is not treated in a timely manner. In most cases, these are irreversible consequences that are attempted to be treated surgically.
Drug therapy for conjunctivitis caused by chlamydia is:
- a weekly course of antibiotics (“Levofloxacin”);
- applying erythromycin ointment several times throughout the day;
- eye drops "Oxial".
Treatment of chlamydial conjunctiva in a child with weak positive dynamics can last until complete cure for 3-4 months.
Causes of conjunctivitis in newborns
An infected mother or maternity hospital staff can infect only a born child due to non-compliance with antiseptic rules.
The risk group includes newborns whose mothers suffer from gonorrhea, trichomoniasis, and chlamydia. Factors contributing to the development of pathology are:
- weak immunological activity in the baby;
- specific structure of the lacrimal canal and visual apparatus: defect or narrowness of the nasolacrimal canaliculus, excessive blood supply to the mucous membrane.
Due to the factors described above, purulent conjunctivitis is especially common in children under one year of age, and develops against the background of blockage of the nasolacrimal duct (dacryocystitis).
Varieties and symptoms
Symptoms depend on the type of bacteria. General signs:
- inflammatory process in the eyes: itching, burning, redness, swelling;
- purulent exudate;
- symptoms of intoxication: irritability, weakness, fever.
Staphylococcal
Staphylococcal conjunctivitis is the most common. Infection occurs in the maternity hospital or through communication with a sick person or animal.
It begins acutely, affecting both eyes simultaneously. The mucous membrane swells and turns red, and pus discharge appears. After sleep, they dry out on the edges of the eyelids, making it difficult for the child to open his eyes.
The pathology, although accompanied by severe discomfort, is treated easily and quickly. Blepharitis often develops in parallel.
Chlamydial
Usually occurs in a chronic form. The mucous membrane becomes dark red in color, and roughness can be seen on its surface. Subsequently, ulcers appear, from which pus comes out.
Gonococcal
It is typical for newborns whose mothers suffered from acute gonorrhea during pregnancy and childbirth. The first signs appear three days after birth. First, the eyes swell, the eyelids become red and thickened, and the conjunctiva becomes loose.
After some time, the swelling subsides and yellowish purulent mucus begins to come out of the eyes. The discharge is thick and viscous.
Gonococcal conjunctivitis is dangerous by spreading to the cornea and developing an abscess. For the purpose of prevention, babies in the maternity hospital have their eyes instilled with disinfectant solutions.
Sometimes older children become infected with gonococcal conjunctivitis from a person with gonorrhea. In this case, the symptoms of the disease are similar.
Pseudomonas
Usually the disease is caused by wearing dirty contact lenses and improper care of them, and the use of non-sterile medications.
This form is accompanied by severe swelling, redness and loosening of the conjunctiva. The purulent exudate is not abundant and has a greenish-blue tint.
Symptoms can be either pronounced or not very pronounced. The danger of the disease is that it can spread to the cornea and lead to permanent deterioration of vision, even blindness.
Treatment is difficult, since Pseudomonas aeruginosa is resistant to most types of antibiotics.
Epidemic
Caused by the Koch-Wicks bacillus, which is carried by flies. Infection occurs through contact.
The disease begins with severe swelling of the eyelid and redness of the eyes. On the second day, copious purulent discharge begins. When they dry, they glue the eyelids together. General symptoms develop: loss of strength, fever, headache.
Complications
Treatment of purulent conjunctivitis in children should begin as early as possible. Otherwise, acute inflammation will become chronic and will bother the baby for a long time. The chronic form is fraught with the formation of scars on the cornea, which causes visual acuity to decrease.
Other complications include:
- eversion of eyelids;
- spread of infection to the deep layers of the eye with the development of abscess, phlegmon, meningitis;
- transfer of the disease to the cornea, blindness.
Etiology
The etiology of this pathological process is well studied. The development of bacterial conjunctivitis in a child can be caused by the following:
- the presence of purulent-septic ailments - otitis media, sinusitis, tonsillitis;
- mechanical damage to the eye;
- too weakened immune system;
- allergic diseases;
- frequent viral illnesses;
- the mother has a sexually transmitted disease (conjunctivitis in a newborn);
- the reaction of the child’s body to long-term use of medications.
It should be noted that conjunctivitis in a child against the background of previous viral or chronic diseases can only occur if the immune system is severely weakened.
Treatment methods
Doctors prefer to treat purulent conjunctivitis comprehensively. For mild cases, the use of local drops and ointments is sufficient. These are mainly antibiotics that block the action of the pathogen and suppress inflammatory processes.
Principles of therapy
To maximize the effect of treatment, follow the clinical recommendations:
- Flush the child with gas before using medications. The purulent exudate contains a lot of pathogenic flora. If it is not removed, treatment will be ineffective;
- wash your hands well before and after using eye drops;
- In case of severe lacrimation, instill eye drops more often, as the drug is quickly washed out from the conjunctiva. The dosage and frequency of use should be discussed with your doctor;
- treat both eyes, even if only one is affected;
- for rinsing, use sterile cotton wool or tampons - new for each eye;
- If the doctor has prescribed an ointment, it is best to apply it before the child goes to bed.
Treatment regimen at the initial stage
If the disease has just begun and has not yet fully manifested itself, you can get rid of it very quickly. For first aid, the ophthalmologist prescribes:
- washing the eyes with a weak solution of manganese;
- tetracycline ointment;
- Levomycetin drops.
The treatment regimen is as follows:
- After sleep, the baby’s eyes are wiped with a swab dipped in a manganese solution. Accumulated pus is removed from the outer to the inner corner using a syringe without a needle or a medical bulb;
- the lower eyelid is pulled down and one drop of Levomycetin is instilled. The procedure is carried out hourly;
- if pus is released during the day, it is removed and the eye is washed;
- Before going to bed, tetracycline ointment is placed behind the baby's lower eyelid.
Treatment after symptoms subside
After the discomfort in the eyes goes away and the amount of pus secreted decreases, the number of instillations is reduced to 2-4 times a day, and ointment is applied once before bedtime.
Therapy continues until symptoms disappear completely and for several more days after recovery. This is necessary to completely neutralize pathogenic microflora and minimize the likelihood of relapse.
Eye drops
How to treat conjunctivitis with purulent discharge? Doctors prescribe gentle antibiotics for children that do not cause irritation:
- Levomycetin. Suitable for children from birth, does not cause side effects.
- Albucid. Doctors prefer this drug for the absence of chemical compounds in its composition and the minimum number of unwanted reactions. The duration of therapy is limited to one week.
- Tobrex. A broad-spectrum antibiotic, effective for most types of purulent conjunctivitis.
Sometimes ophthalmologists prescribe Oftadec, but it requires careful adherence to the dose prescribed by the doctor.
Ointments
Ointments have a more concentrated composition, so using them once or twice a day is sufficient. It is best to carry out the manipulation at night. The ointment creates a protective film on the surface of the conjunctiva that has a therapeutic effect.
For children, tetracycline ointment, Floxal, is usually chosen.
Solutions
Used to wash and disinfect eyes. In addition to manganese solution, the following are allowed:
- Furacilin solution;
- decoctions of medicinal herbs (chamomile, calendula flowers, sage);
- ready-made pharmaceutical products: Miramistin, Vitabact.
Features of treatment of staphylococcal infection
The symptoms of this purulent conjunctivitis, caused by contact with the mucous membrane of staphylococcus, appear first in one eye, then, after 2 days, in the second.
Pathology manifests itself as follows:
- itching and burning occurs;
- photophobia appears;
- swelling of the eyelids;
- increased production of mucous secretion.
Purulent mucus during staphylococcal infection, actively produced at night, prevents the free opening of the eyes in the morning. Drying on the eyelashes, it causes a lot of discomfort to the baby.
If the above symptoms appear, it is imperative to show the child to an ophthalmologist, who, having identified the pathogen, will prescribe appropriate treatment.
Antibacterial therapy is the purpose of:
- drops (“Floxal”, “Tobrex” or “Okacin”) – most often one drop is used in each eye in the morning and evening;
- ointments (tetracycline or erythromycin) - apply at night.
Treatment rarely lasts more than 10 days. The prognosis of the disease is favorable. To prevent re-infections, it is extremely important to pay great attention to the child’s hygiene.
Advice from Dr. Komarovsky
The pediatrician advises contacting an ophthalmologist at the first symptoms of the disease. In this case, treatment will be quick and effective.
You should not self-medicate, apply lotions or compresses to the child’s eye. This promotes the spread of bacteria and worsens the disease.
It is very important to establish the type of conjunctivitis, since the treatment regimen depends on this. For example, allergic and viral forms do not require the use of antibiotics. And purulent, caused by bacteria, can only be treated with their help.
Diagnostics
If you suspect conjunctivitis in a newborn or older child, you should immediately consult an ophthalmologist. After a personal examination, the doctor may order additional tests or immediately prescribe the correct course of treatment. To clarify the diagnosis, the doctor may prescribe the following instrumental research methods:
- serological test;
- cultural research method;
- PCR.
Based on a personal examination, anamnesis assessment and the results of the study, the correct course of treatment is prescribed.
Prevention
To minimize the risk of purulent conjunctivitis in a child, follow these simple rules:
- teach your child not to touch his eyes with dirty hands;
- disinfect toys;
- regularly ventilate the room where the child is located, humidify the air;
- provide your baby with individual household items;
- change the bedding on which the child sleeps more often;
- strengthen your immune system. Proper nutrition, vitamin complexes, an active lifestyle, and hardening procedures will help with this.
Purulent conjunctivitis is an unpleasant disease that causes severe discomfort to children. To quickly get rid of it and prevent complications, strictly follow all the recommendations of your doctor and do not self-medicate.